Post-COVID-19: How to Reform Egypt Health System?
The World Health Organization (WHO) states that the health system consists of all the organizations, institutions, resources and people whose primary purpose is to promote, restore and/or maintain health; and that such system needs staff, funds, information, supplies, transport, communications and overall guidance and direction to function. The actions of the health system should be responsive and financially fair, while treating people respectably. Also, a good health system is one that contributes to improving people’s lives tangibly day after day, where the primary responsibility for the overall performance of a national health system rests with the government. WHO also emphasizes that strengthening health systems and making them more equitable is one of the basic strategies for combating poverty and promoting development[1].
As for the concept of public health, it is defined by the American Centers for Disease Control and Prevention (CDC) as the science of protecting and improving the health of people and their communities. This work is achieved by promoting healthy lifestyles, researching disease and injury prevention, and detecting, preventing and responding to infectious diseases. Also, public health works to limit health disparities and promote healthcare equity, quality and accessibility.
The essential difference between the concept of public health and the clinical treatment by doctors and nurses, is that physicians primarily focus on treating individuals after they become sick or injured. As for the public health, it is concerned with all the health, environmental and societal aspects that lead to occurrence of the disease, and it tries to prevent problems from happening or recurring through implementing educational programs, recommending policies, administering services and conducting research, related to the healthy lifestyle[2].
First: identifying the problem and gathering evidence
The Egyptian health system suffers from multiple problems, due to the political system’s lack of interest in the health component and its failure to place it on its priority agenda, as it gives priority to spending on security and military institutions rather than spending on service institutions, mainly in the area of health and education, which has led to deterioration of health services and a drastic decline in health spending over the past four decades.
The key weaknesses of the Egyptian health system include:
1- Expenditure and funding sources
In terms of the financing philosophy of the Egyptian health system, it can be classified as being based on the “out-of-pocket model”, the most widespread model in the world, as there are approximately 40 advanced countries that have been able to integrate into the three above systems. All the remaining world countries, not less than 160, that suffer from many development problems related to poverty, unemployment and low level of education, follow this model (out-of-pocket model), based on the fact that ‘the rich get health care and the poor get sick or die’[3].
While discussing the strategy of developing health policies, known as the ‘White Paper’, by the Supreme Council of Health in 2014, former Minister of Health Adel Adawi, indicated that the decrease in government spending on health over long years led to incurring citizens about 72% of the total health spending from their own resources. This has been evident in the increased dependence on the private sector with respect to provision of health services[4].
The reason for the low government spending on the health sector is due to several reasons, including the high prices of medicine, the high cost of treatment in private hospitals, and the high prices of medical examination in private clinics, whereas the services provided by the government are limited, and that the Public Authority for Health Insurance provides health services to only 8% of citizens, despite the fact that it covers more than 60% of the population[5].
The decline in the State’s role in spending on the health sector and the maximization of the role of private hospitals have caused a major crisis after the outbreak of the COVID-19 epidemic in Egypt, because the Ministry of Health was unable to impose a fixed price for treating citizens infected with COVID-19 on these hospitals. Moreover, private hospitals threatened the Ministry of Health that they would stop providing the service in the event that the ministry sought to impose a compulsory pricing on the medical service that they provided related to the COVID-19 patients.
2- Human resources
The health system in Egypt suffers from a severe shortage in doctors, especially in vascular, anesthesiology, emergency, and fever specialties. According to a study prepared by the Supreme Council of University Hospitals and the Ministry of Health’s technical office titled: “Labor Market Needs of Medical Professions in the Next 5 Years, As of 2020”, the number of registered human doctors who have got a license to practice the profession, excluding the pensioners, is 212,835 doctors, of whom only 82,000 are currently operating in all health sectors, by 38% of the number of registered doctors who have a license to practice the profession, either working in hospitals affiliated with the Ministry of Health, government university hospitals, or the private sector.
Comparing the number of doctors currently working in the health sectors and the number of doctors registered or licensed to practice the profession from the Egyptian Medical Syndicate, we find out that 62% of them work overseas, where they either had resigned from government work or obtained unpaid leave before traveling for work abroad. The study concludes that Egypt has a doctor for every 1162 citizens, while the global average according to the World Health Organization is one doctor for every 434 citizens[6].
As for nursing, the total number of the nursing staff that were actually working in the government sector was 187,090 in 2016[7], according to a Central Agency for Public Mobilization and Statistics (CAPMAS) bulletin issued in 2017, while the CAPMAS bulletin issued in November 2019 confirmed that the total number of nurses operating in government hospitals was equivalent to one nurse per 688 citizens, which means that the nursing rate represents 1.45 nurses per 1000 citizens, as confirmed by the World Bank report[8].
3- Problems of the infrastructure of government-owned health institutions in Egypt:
A- The problematic of diversity:
There is a large network of government hospitals in Egypt, each has its own regulations, budget, and sometimes the level of its visitors. Also, there are differences in the financial regulations for the provided medical service, where some hospitals, such as hospitals of the Secretariat of Specialized Medical Centers, follow regulations similar to those of private hospitals.
Consequently, the official health system in Egypt is not limited to the hospitals of the Ministry of Health only, but there are also the university hospitals, the armed forces hospitals, and the health ministry hospitals, including public and central hospitals, health insurance hospitals, hospitals of the Secretariat of Specialized Medical Centers, hospitals of the Hospitals and Educational Institutes Authority, and Mental Health Secretariat hospitals.
B- The problem of the weakness of the health insurance system:
Military personnel are treated inside armed forces hospitals, while personnel of the judiciary, financial institutions, such as Egyptian Tax Authority and the Ministry of Finance, the electricity, petroleum, and communications companies, and others, contract with private insurance companies that provide them with health insurance services in private hospitals. Meanwhile, the personnel of the service institutions are treated at hospitals of the General Health Insurance Authority, where hospitals provide poor a medical service due to their limited potentials. The rest of the Egyptian people are treated through the system of ‘treatment at the State’s expense’ at the hospitals of the Ministry of Health and the university hospitals.
C- The problem of the expansion of the private sector
The private sector controls more than 70% of investment returns within the health sector in Egypt, due to the citizen’s loss of confidence in the quality of medical services provided by government hospitals. Reviewing the map of the 1848 hospitals operating in the Egyptian health sector in 2018, the private sector acquired 1157 hospitals, at a rate of 62.6%, while government sector hospitals accounted for 37.4%, including general, central and government hospitals, with a total of 691 hospitals[9].
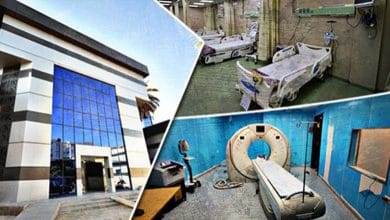
D- The problem of the dilapidated structure of government hospitals
According to Hisham Atta, the former head of the Ministry of Health’s curative medicine sector, the poor medical service provided to citizens in hospitals is due to deterioration of the infrastructure of more than 30% of these hospitals[10]. Also, the Ministry of Health hospitals suffer from recurrent crises and sometimes complete or partial closure due to maintenance contracts. Some hospitals are closed for a period of ten years for replacement, renewal or reconstruction. A report by Al-Bawaba News in April 2017 noted that 186 general and central hospitals and health units were suspended due to maintenance or reconstruction work. Also, Mona Mina, Secretary General of the Egyptian Medical Syndicate revealed that 2016 witnessed the closure of 450 health units in various Egyptian governorates[11].
E- The problematic of the shortage of intensive care rooms
Egypt suffers from a severe shortage of intensive care beds. According to a recent statement by Sherif Wadei, advisor to the Minister of Health for care and emergency, Egypt has 5,600 intensive care beds in various government university hospitals, hospitals affiliated with the Ministry of Health, the armed forces, and the police[12]. Hussein Khairy, the head of the Egyptian Medical Syndicate, also confirmed that hospitals are in a real crisis, due to the scarcity of intensive care beds and incubators, which have affected thousands of patients and their families, and even doctors, who often resort to postponing some operations. Khairy called on Abdel Fattah Al-Sisi to adopt an initiative to cover the deficit of intensive care rooms and incubators[13].
As for ventilators, according to Nader Saad, the Council of Ministers’ spokesperson, the Ministry of Health has only 4,000 ventilators[14], while Hala Zayed, Minister of Health, confirmed that the occupancy rate of ventilators in Cairo reached 97% in June, before the rate fell in July, after the decline in the number of infected cases[15].
4- The preventive component
The preventive component is considered one of the most important weaknesses in the Egyptian health system, for several reasons, most prominently the focus of health policy-makers in Egypt on the curative component, considering that it is the tangible component through which the official can be evaluated, with respect to establishment of hospitals or development of departments. On the contrary, spending on the preventive component requires a different culture and community awareness. Some officials may fear of likely accusations of wasting public money in the event of expansion of spending on the preventive sector.
In a previous study titled, “Is Egypt likely to become an endemic focus of coronavirus?”, the researcher addressed the weaknesses of the preventive component of the Egyptian health system, represented in the endemicity of the Hepatitis C viral infection in Egypt, where Egypt included the highest infected cases the virus in the world, as well as the endemicity of bird flu and the swine flu. Egypt also suffers from a decline in infection control indicators in hospitals, which led to exposure of many doctors and members of the nursing staff to contracting Virus C, as well as kidney failure. Egypt suffers from a structural defect with regard to interest in fever hospitals, which resulted in the closure of 70 fever hospitals by a decision from former Health Minister Hatem El-Gabaly, in addition to the dilapidated infrastructure of the remaining fever hospitals, most notably the Abbasid fever hospital and the Imbaba fever hospital, which resulted in failure of fever hospitals in Egypt to be designated for isolation of COVID-19 cases[16].
Second: Identifying concerned parties
In view of the broad concept of public health as a way of healthy life, there is expansion in the size of the concerned parties, including government bodies, community bodies, or even religious bodies. Following are the key bodies concerned with improvement of the society’s public health:
1- The Ministry of Health, as the executive body mandated constitutionally to preserve the life of Egyptian citizens, and assigned to ensure provision of their right to treatment and access to medicine and other health services, such as vaccinations, preventive measures, family planning services, and psychological support.
2- The Egyptian Drug Authority (EDA), as the authority responsible for preserving the quality and efficacy of the drug, registering the drug in the Egyptian market, and setting up general policies to ensure fair availability of medicinal products to citizens.
3- The National Food Safety Authority (NFSA), as the authority responsible for setting binding rules that guarantee food safety, where all public and private food establishments are subject to the authority’s control. It also undertakes healthy food education and contacts with officials, consumers, food handlers and producers in order to ensure the quality and safety of food to preserve public health.
4- The Ministry of Environment, as the competent authority to reduce the current rates of pollution to preserve public health and improve the quality of life, as well as supporting integrated environmental management systems to provide a healthy environment for citizens[17].
5- The Parliament, as the legislative body entrusted with drafting laws and legislation that contribute to activating the role of the executive authorities, defining the terms of reference and organizing interrelations to ensure efficiency, effectiveness and development of performance, in a way that achieves balance, effective oversight and accountability, and guarantees the security and safety of the citizen’s health.
6- The Ministry of Education, which is supposed to carry out the healthy upbringing process, and raising students’ awareness about hygiene, prevention methods and healthy eating, as well as awareness about the dangers of viruses and the importance of sports and the proper construction of the body.
7- Research centers, which should play a major role after the coronavirus crisis, whose repercussions included all aspects of economic, political and social life. The research centers have to pay attention to health economics and the study of various health systems, and public policies related to the health sector.
The researcher would like to point out that the area of public health is more extensive and comprehensive, including many governmental and civil bodies, as it comes within a series of many measures related to the quality of education, fighting poverty and combating illiteracy, as well as building a strong health system and policies, existence of a comprehensive program for health insurance, supporting the preventive system, provision of medicine, and food safety .
Third: Available alternatives
(A) The alternative proposed by the government:
The government has presented the alternative that we referred to in the executive summary, that is based on establishment of a health system relying on the concept of universal health coverage for all citizens through presence of permanent financing sources, a system that is currently adopted through the experience of comprehensive health insurance in Port Said.
(B) The system based on the public health approach:
The system based on the public health approach is a more comprehensive and extensive system, as it is concerned with other non-curative components, related to the preventive aspect, health culture, environmental and societal factors, proper nutrition, attention to immunity, promotion of the culture of social distancing and preventive precautions, and development of early warning systems in the event of epidemics or viral outbreak in a specific area.
To compare the two models, the researcher designed the following table that summarizes the pros and cons of both approaches.
Table (1) Comparison between pros and cons of health reform approaches:
|
|
Comprehensive Health Insurance |
Public Health Approach |
|
PROS |
1- Comprehensive health coverage for all citizens is one of the most important advantages that enables any society to face disasters and health crises. 2- Putting an end to the waiting lists that Egypt suffers from as a result of the absence of health insurance coverage. 3- Development of the infrastructure and medical devices in government-owned hospitals and provision of appropriate medical supplies and medicines. 4- Improving the medical services provided by the State in general. |
1- Paying attention to the preventive component along with the curative component. 2- Providing great opportunities for State institutions and civil society to work within the public health system, given the broad and comprehensive approach of public health. 3- Improving all components of society due to working in a parallel line, which guarantees facing the societal problems related to public health, such as poverty, ignorance, pollution and bad eating habits. 4- Raising the community awareness to ensure the ability to face crises, disasters and epidemics, with the least losses. 5- Expansion of the concept of defining health from being merely absence of pain and disability, to new horizons according to the WHO definition as “a state of complete physical, mental and social well-being and not merely the absence of disease or infirmity”.[18] 6- Strengthening the immune system starting from childhood.
|
|
CONS |
1- The implementation period is long as it extends to 15 years. 2- There is a stumbling in the implementation of the first phase. Although the actual implementation of the project was scheduled for mid-2018, however, it started in mid-2019. Moreover, the implementation was not carried out in some scheduled governorates of the first phase, such as Luxor and North Sinai – due in early March 2020 – because of the coronavirus crisis. 3- It does not care about preventive aspects, and fever hospitals have not been included in the project. 4- There is lack of clarity regarding the basic care units, as part of them will follow the new system as the cornerstone of its implementation, depending on the family doctor, and the other part will follow the Ministry of Health to provide preventive services, which will cause problems among workers in the same place, given the fact that they follows various financial regulations. 5- It cannot address large-scale epidemics such as coronavirus, as it focuses on the curative part only. 6- It does not include university hospitals, more than 110, while it opened the way for private hospitals to manage the project. |
1- It needs a society with a high level of culture, awareness, and education 2- It requires a long time for achievement, as it may take up to 20 years. 3- Implementation requires coordination, but there is lack of coordination between State institutions in Egypt. 4- It requires a high financial cost, largely borne by the State, as it cannot be borne by the citizen, as it happened in the comprehensive health insurance project.
|
|
Proposed Solutions to Overcome Obstacles |
1- Inclusion of preventive sector services within the new system. 2- Inclusion of fever and chest hospitals in the comprehensive health insurance. 3- Inclusion of university hospitals in the new health insurance project. 4- Development of an early warning system to detect infectious diseases
|
1- Development of awareness and spread of culture about the significance of health and its impact on all walks of life. 2- Teaching a course on public health in schools and universities. 3- The State and society should accept the idea of the need to spend much on education and health education although they do not have quick tangible results on the ground. |
Source: the researcher’s work
Fourth: Criteria of differentiation between proposed policies
1- The health promotion criterion
The health promotion criterion is considered one of the important criteria set by the World Health Organization, defining it as: “Health promotion enables people to increase control over their own health. It covers a wide range of social and environmental interventions that are designed to benefit and protect individual people’s health and quality of life by addressing and preventing the root causes of ill health, not just focusing on treatment and cure.”[19] The health promotion criterion relies on health policies that ensure existence of three key elements, namely, good governance for health, health literacy, and healthy cities, based on healthy urban planning and building up preventive measures, and primary health care facilities.
2- The IPC criterion
The infection prevention and control (IPC) criterion provides the potentials and measures to prevent infection and control it. According to the definition of the World Health Organization, it is “a scientific approach and practical solution designed to prevent harm caused by infection to patients and health workers … IPC occupies a unique position in the field of patient safety and quality universal health coverage since it is relevant to health workers and patients at every single health-care encounter.”[20]
3- The criterion of fair and comprehensive health services coverage
The criterion of fairness in obtaining health and medicinal services is one of the criteria that has strongly emerged in light of the coronavirus crisis, along with the universal health coverage. The researcher believes that emergence of these criteria will place a greater burden on governments to formulate policies for health economics, based on fairness and social inclusion, not on profit-making and private investments.
Fifth: Comparing available options
Based on the above analysis, the researcher believes that the second approach, that is adoption of the “public health approach”, is the best option for reforming the Egyptian health system, for several reasons, including:
1- The coronavirus crisis has demonstrated the inability of the traditional health systems to withstanding epidemics, amid its weak control of viruses, and that focus on the curative component only has not succeeded to address and control the crisis, even in countries that have advanced health systems.
2- The need to establishing a new health system that must be flexible and able to address unexpected and sudden mutations that may cause a global epidemic, paying attention to both the protective and curative components.
3- The public health approach provides community education, communication, and health literacy, which contributes to providing a fair distribution of curative, medicinal and preventive services.
4- The health system that relies on the public health approach addresses multiple aspects of health well-being based on the physical, mental, social, emotional and spiritual components, which contributes to development of the health system as well as the service provider’s style.
5- The concept of public health expands to include marginalized and vulnerable groups, as it is concerned with the immunity and health conditions of the mother and the fetus, facing poverty, slums, environmental pollution, delinquency and crime, as well as addressing aging, and increasing man’s average lifespan.
6- The public health approach is considered a way of life, as it has multiple manifestations and patterns, including medical, cultural, social, sports, and preventive components brought together, to ultimately achieve the goal of health promotion.
7- The public health approach maximizes the community’s ability to take precautionary, preventive and regulatory measures that would contribute to reducing the severity of epidemics, addressing them and preventing their rapid spread.
8- This approach reduces the exposure of health sector workers to infection and contraction of viruses, and thus reduces the death rates among members of the medical team.
Conclusion
The crisis of the coronavirus pandemic has highlighted the inability of traditional health systems to withstand the outbreak of epidemics, due to several factors, most prominently the ease, speed and intensity of people’s movement between countries of the world, thanks to the great development of global transport, where the role of the traditional health system was restricted to reaction and pursuit of withstanding the pressures and avoiding collapse. This resulted in invocation of reform ideas related to the need to give the preventive component a major role in building the new health system, as well as paving the way for formation of social protection networks that would be able to organize society in times of epidemics.
The exacerbation of the coronavirus has also led to rising debate about the importance of the universal coverage of medical service including all citizens, the fair distribution of these medical services, the central role of the State in the health system reform, and avoiding commodification of medical services. Accordingly, the most appropriate approach has become to create a new health system based on a more broad concept that would include the preventive component along with the curative component, where the management of the health file would not be restricted to only the ministry of health; but the ministry of health would only be part of the whole system.
Egypt Health System
Footnotes
[1] World Health Organization, Link
[3] P N H P, Health Care Systems – Four Basic Models, Link
[4] Al Mal newspaper, August 21, 2014, Launch of the White Paper program to start health strategies for the coming years, accessed 2020, Link
[5] Asmaa Sorour (Interview), January 4, 2013, In interview with Al-Shorouk: Assistant Minister of Health .. treatment at the expense of the State to be cancelled after applying the health insurance system, accessed 2020, Link
[6] Mohamed Waheed, June 20, 2019, the continued crisis of shortage of doctors. 62% of them work overseas, Al-Bawaba News, accessed 2020, Link
[7] CAPMAS, Egypt Bulletin in Figures – Health 2018, Link
[8] CAPMAS, Annual Bulletin of Health Services Statistics 2016, November 2017, Link
[9] Ahmed Awaad, June 10, 2020, After the PCR price crisis: How much do private hospitals represent from the health sector in Egypt, Al-Mal newspaper, Link
[10] Asmaa Sorour and Yasmine Abdel Razek, Head of the Clinical Medicine Sector to Al-Shorouk: The infrastructure of 30% of governmental hospitals is dilapidated, Al-Shorouk newspaper, accessed 2020, Link
[11] Walid Salam, April 4, 2017, Hospitals inhabited by neglect. 186 hospitals out of service for maintenance or reconstruction, Al-Bawaba News, Link
[12] Hossam Emad, June 1, 2020, Health Ministry: We have used 10% of the intensive care beds since the start of the COVID-19 pandemic, al-Shorouk Gate, Link
[13] Egyptian Medical Syndicate (EMS), quoting Al-Masry Al-Youm, February 6, 2020, Head of EMS Hussein Khairy: We need a presidential initiative to support intensive care units and incubators, Link
[14] Mohamed Khamis, May 21, 2020, The cabinet reveals number of Health Ministry’s intensive care beds, Masrawy, Link
[15] Minister of Health: Occupancy rate of ventilators was 97% a month ago, Al-Wafd, July 18, 2020, Video, Link
[16] Amgad Hamdi, Egyptian Institute for Studies, Link
[17] Egyptian Ministry of Environment website, Link
[18] World Health Organization, What is the WHO definition of health? Link
[19] World Health Organization, What is health promotion? Link
[20] World Health Organization, Infection prevention and control, Link